Depression
Mental Health and Trauma in the Juvenile Justice System — Relias Webinar on May 21
Today is Children’s Mental Health Awareness Day
Elwood Watson: Men and Mental Health
Sen. John Fetterman on Depression, Recovery, and “Making Up Any Lost Time”
Concern Grows in Schools for Mental Health, ‘Erosion of the Social Fabric’
October 3–7 is Mental Illness Awareness Week
National Report: Worker Anxiety, Depression Surging
The National Alliance for Direct Support Professionals (NADSP) shared this report:
Direct Support Workforce and COVID-19 National Report: 12-Month Follow-up
While vaccination rates have improved among professionals supporting people with intellectual and developmental disabilities since the early days of the COVID-19 pandemic, their mental and physical health have declined, a new survey shows.
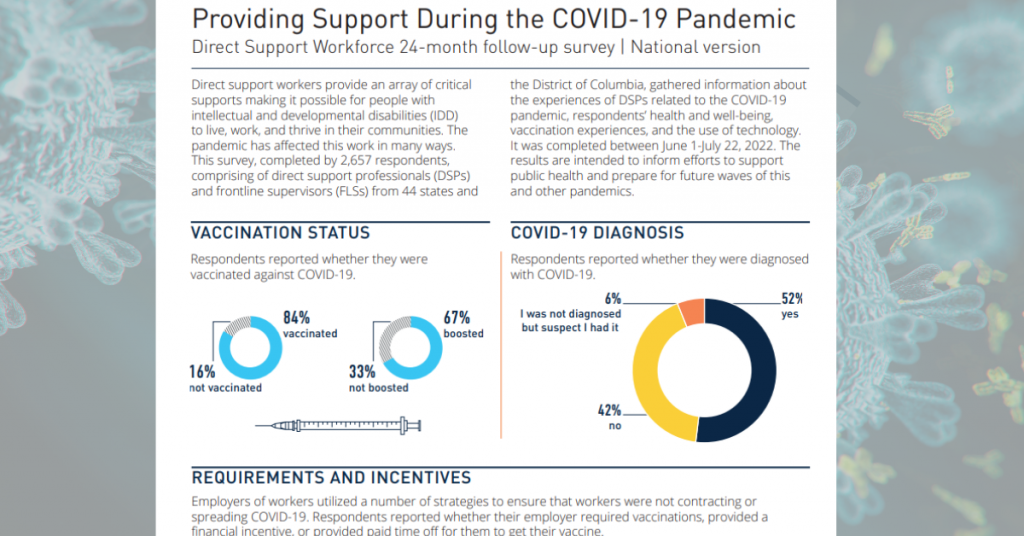
The Institute on Community Integration, in partnership with the National Alliance for Direct Support Professionals (NADSP), surveyed 2,657 DSPs and frontline supervisors about their experiences supporting people with IDD during the pandemic. The newly released survey report is a 24-month follow-up to an initial report issued in April 2020. Additional surveys were conducted six and twelve months after the initial report. The survey series represents the largest-ever national study of the DSP workforce.
According to the report, 52% percent of DSPs reported being diagnosed with COVID-19, and 6% were not diagnosed but suspected they had it. Among employers, 65% did not require DSPs to be vaccinated.
Sixteen percent of DSPs remain unvaccinated. Of the 84% who are vaccinated, 67% reported having at least one booster shot.
While vaccination rates have improved from the 12-month survey in 2021 (from 72% to 86%), the mental wellbeing of DSPs has declined. Forty percent of DSPs reported experiencing depression, compared with 36% one year ago; 43% had difficulty sleeping, a 13% increase; and 56% reported increased anxiety, a 14% increase. Fifty-nine percent of respondents said they felt pressure to work extra hours.
“Direct support professionals and frontline supervisors have worked as hard as they can,” said Amy Hewitt, ICI director and lead investigator of the study. “This survey shows that their mental health is worsening, and we don’t have the resources to address it. Working this much overtime is not sustainable.”
A national plan to increase the size of the direct support workforce would help to alleviate multiple troubling issues, Hewitt said.
“This workforce has been overlooked and in crisis for years, with high turnover and vacancy rates, low wages, and lack of access to affordable benefits,” she said.
More than half of DSPs receive government-funded assistance, such as housing, energy, food, and healthcare. The pandemic made staffing even more difficult, increasing stress, expectations, and risk on those who remain in their positions.
The 24-month follow-up survey also looked at changes in technology use during the pandemic. Fifty-nine percent of DSPs reported using technology more or a lot more than before the pandemic. Thirty-six percent of the respondents said the use of technology had a somewhat positive impact on their work, and 14% reported it had a very positive impact. Seventeen percent reported a somewhat negative impact and 3% a very negative impact.
Read the full report, a short version, and select state-specific versions here.
Please contact Jerry Smith with questions.
“Together for Mental Health” — National Alliance on Mental Illness Recognizes Suicide Prevention Awareness Month
OMHSAS Releases MH Bulletin for Older Adults
The Office of Mental Health and Substance Abuse Services (OMHSAS) is pleased to announce the issuance of Bulletin OMHSAS-22-06 titled “Revised Bulletin for Services to Older Adults.”
In 2019, Pennsylvania ranked 7th in the United States for the largest number of adults 65 and older. In the U.S., between 2020 and 2030, the number of older adults is projected to increase by almost 18 million, a 39% increase. The fastest growing segment of the population during the next two decades is expected to be in the age 85 and older group. Social isolation and limited access to supports negatively impact the well-being of older adults.
Depression, anxiety, addiction, and other mental illnesses are not a normal part of aging and should not be considered as such. As individuals age, the support networks utilized to help manage symptoms of a mental illness may change, resulting in individuals seeking services for the first time in their lives.
The development of depressive disorders occurs frequently in older adults, making it critical that comprehensive mental health evaluations are conducted based on presenting symptoms regardless of age. It is important for providers to evaluate for suicidality given that older adult males have the highest suicide completion rate of any age group.
Older persons diagnosed with a neurocognitive disorder, including dementia, who are experiencing symptoms of a mental illness, including depression, anxiety, substance use disorder, post-traumatic stress syndromes, and behavioral agitation, are guaranteed access to mental health services under laws and regulations of the Commonwealth.
If you have questions or concerns related to this bulletin, please email OMHSAS or contact your RCPA Policy Director.